Eczema and Psoriasis are two skin conditions that are commonly confused with each other, but they are different in many ways. Psoriasis is an autoimmune disease, while eczema is not an autoimmune disease but can be related to allergies. To make it more confusing, psoriasis can often look like eczema which is why they can both be misdiagnosed by medical experts.
Although they can look alike, eczema on a person’s body typically manifests as dry, red patches on the skin. Psoriasis is characterized by raised lesions on the surface of the skin with a silvery-white appearance and is sometimes accompanied by scaling. Eczema usually involves one area of the body whereas psoriasis may involve several different areas.
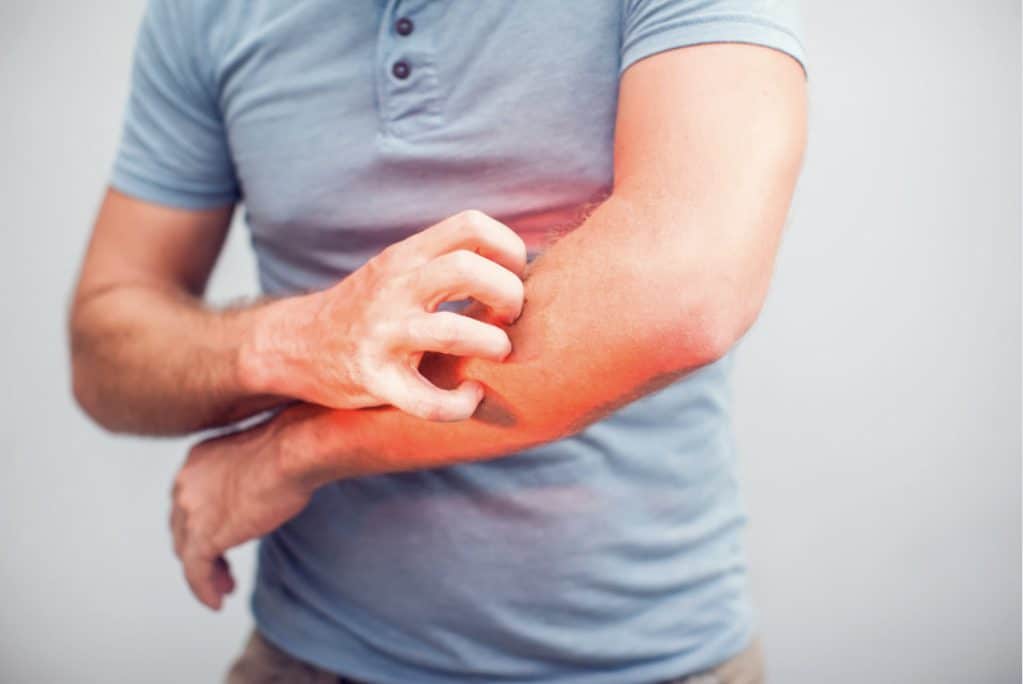
What is Eczema?
Eczema is a chronic inflammatory skin condition influenced by a combination of genetic, immune, and environmental factors. In some individuals, triggers such as allergens, irritants, or underlying imbalances may contribute to flare-ups. When eczema develops, the skin often becomes red, dry, itchy, and cracked.
Eczema is not contagious and commonly affects the face, hands, feet, and elbows, although it can appear anywhere on the body. The severity of symptoms varies from person to person, and treatment approaches are typically tailored to the intensity and frequency of flare-ups.
Eczema-prone skin tends to have a weakened skin barrier, which makes it more difficult to retain moisture. As the skin becomes dry, inflammatory chemicals are released, worsening irritation and leading to intense itching. Scratching may provide temporary relief, but it further damages the skin barrier, creating a frustrating itch–scratch cycle that can be difficult to break.
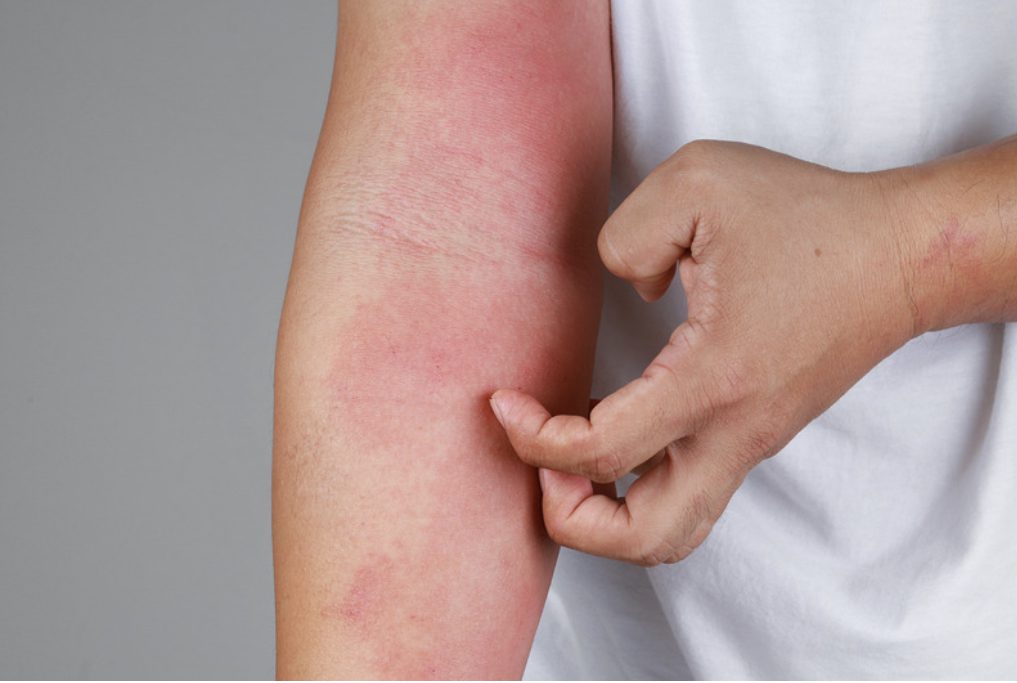
What triggers eczema flare-ups?
Common eczema triggers include stress, harsh soaps, synthetic fragrances, temperature changes, allergens, and disruption of the skin barrier. Because triggers vary by individual, identifying and minimizing personal irritants is one of the most effective ways to reduce flare frequency.
How to Treat Eczema:
There is currently no known cure for eczema. However, symptoms can often be managed and flare-ups minimized with consistent, supportive skincare. A daily routine focused on protecting and restoring the skin barrier is essential for long-term skin health.
Regular moisturizing plays a critical role in preventing dryness and irritation that can trigger eczema flare-ups. Applying a gentle, eczema-safe moisturizer at least twice daily helps maintain hydration and reinforce the skin’s natural protective barrier. It is equally important to avoid products containing harsh chemicals, synthetic fragrances, or unnecessary additives that may aggravate sensitive skin.
Waxelene Aerated Balm helps support eczema-prone skin by deeply moisturizing and protecting the skin barrier. Made with four organic ingredients, it locks in moisture and promotes skin comfort without unnecessary irritants. Its lightweight, aerated texture allows for smooth application while still delivering long-lasting hydration, making it suitable for sensitive skin.
For individuals managing eczema, choosing a clean, non-irritating balm can make a meaningful difference in maintaining healthier-looking, more comfortable skin.
In addition to topical care, it is important to consider internal factors. Emerging research has highlighted the connection between gut health and inflammatory skin conditions, including eczema. The gut-skin axis suggests that imbalances in the microbiome may influence immune responses and skin flare-ups. As a result, strategies such as supporting digestive health through a balanced diet, probiotics, and lifestyle adjustments may complement a comprehensive eczema management plan.
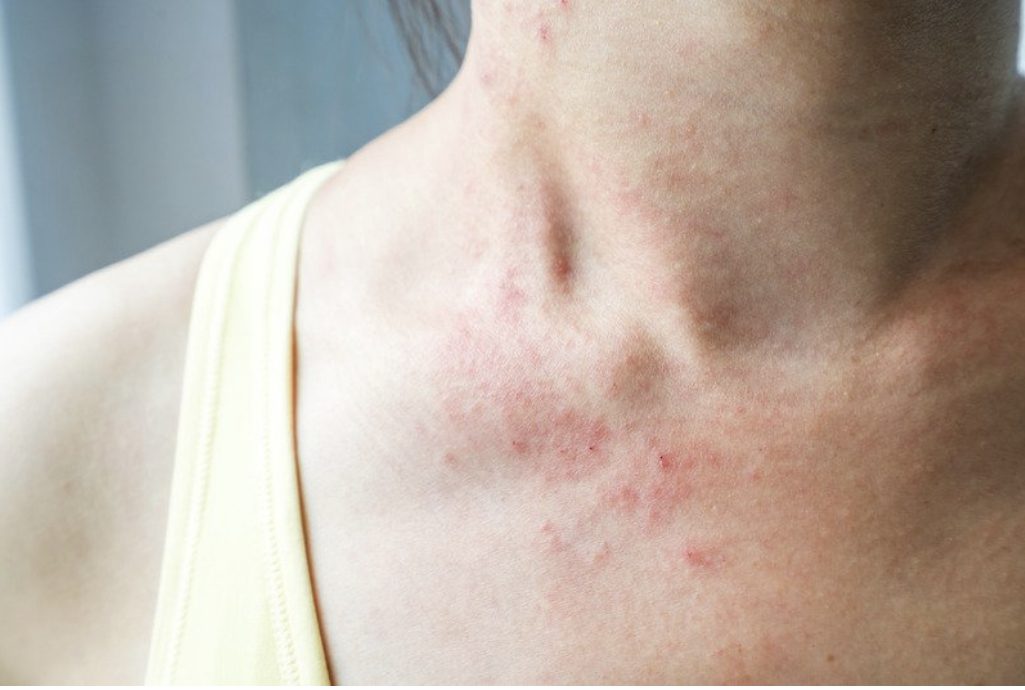
If you think your skin is trying to communicate a gut imbalance you should begin by speaking to your doctor, dermatologist, or naturopath. They may recommend a specific elimination diet to find out which foods are causing your skin to become inflamed. This is a good opportunity to get your gut bacteria back in balance regardless.
What is Psoriasis?
Psoriasis is an autoimmune disease that starts in your genes which causes skin cells to grow too quickly and pile up on top of each other, which can result in patches of red, scaly skin. It can be a very difficult and painful experience for those who suffer from it. There are plenty of treatments that can be used, but it is important to find the one that works best for you.
Psoriasis is not contagious and symptoms can differ from person to person. It has been known to cause dents and discoloration of the nails. Some people also get small, drop-shaped sores on the chest, arms, legs or scalp. Some people even experience swollen, painful joints!
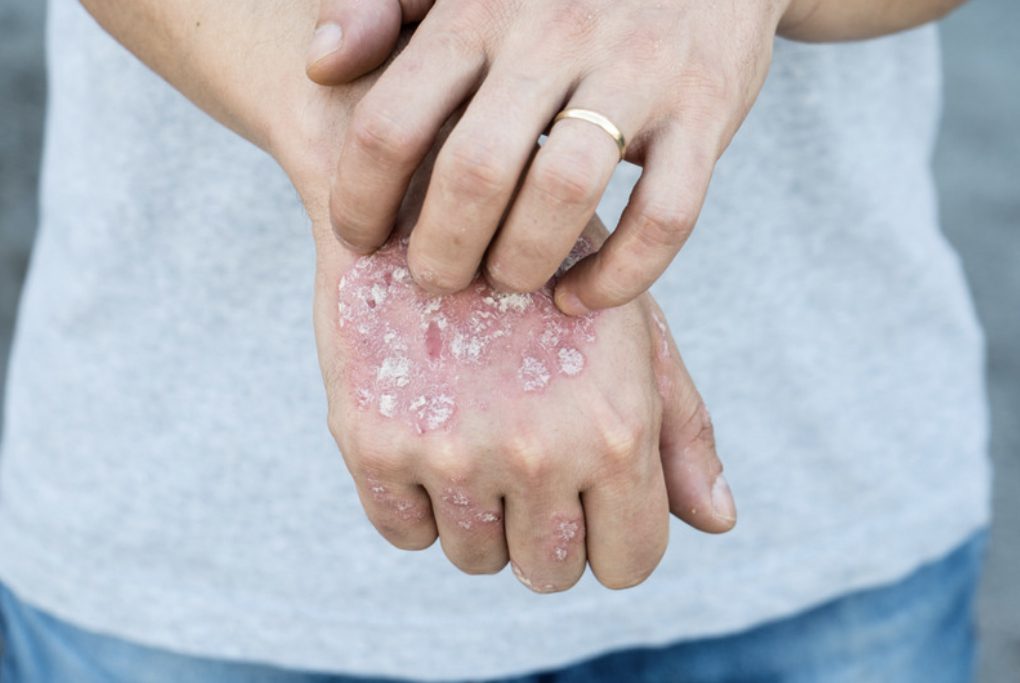
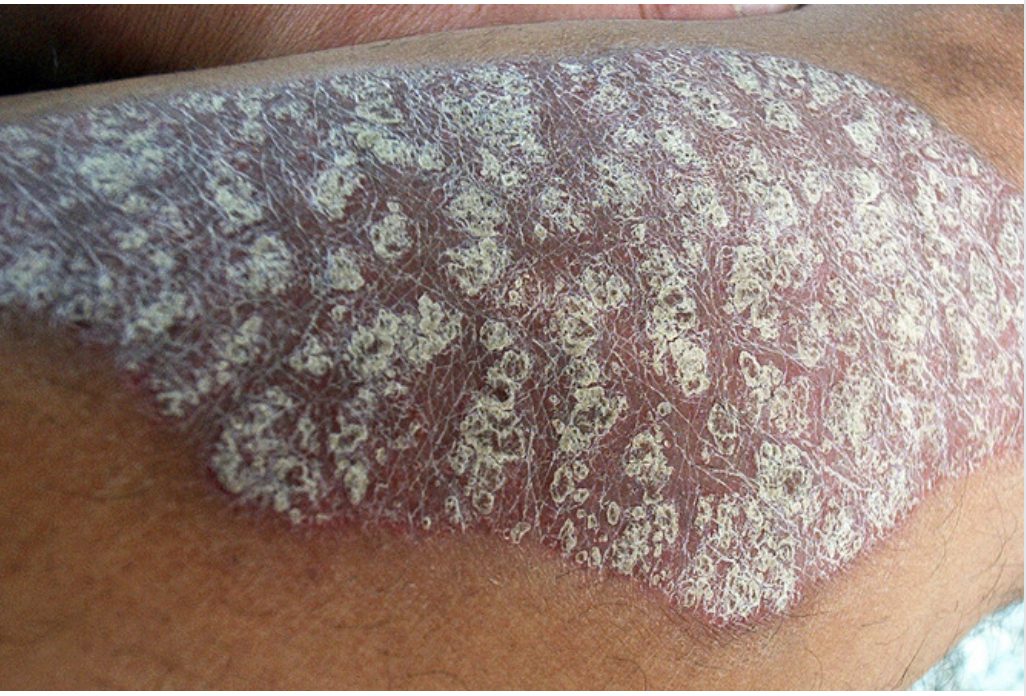
Some people with psoriasis may suffer from what’s known as plaque psoriasis which affects the soles of the feet, hands, and elbows. It can also affect other parts of the body. The skin becomes red and thickened with patches of silvery scales. The cause of plaque psoriasis is not known but it is thought to be due to a combination of genetic and environmental factors. Applying a thick layer of the aerated balm daily will help to rehydrate dry areas.
How To Treat Psoriasis:
The two most common treatments are phototherapy and psoralen ultraviolet A (PUVA). These treatments both use special light directed at the skin to reduce inflammation and clear away scales, respectively.
Phototherapy is a treatment for psoriasis that uses ultraviolet light. It can be done outside, inside on specially-designed equipment, or inside on an artificial light source. It’s also called UVB therapy. Psoralens are medication that is applied to the skin first before the treatment.
PUVA therapy involves taking or applying a medication called psoralen before exposure to UVA light to enhance its effectiveness. Psoralens are plant-derived substances that when combined with UVA, create a chemical reaction that kills the abnormal skin cells responsible for psoriasis.
Psoriasis may also be treated with topical medications such as corticosteroids or coal tar, which help reduce inflammation and pain by reducing the growth of cells in the top layer of skin and trapping fluid between layers.
Other Skin Conditions That Look Similar:
If you are reading this article with the purpose of identifying a mystery rash you may want to consider the other possibilities before self-diagnosing yourself with eczema or psoriasis. Here is a list of some other skin conditions that can be mistaken for eczema and psoriasis.
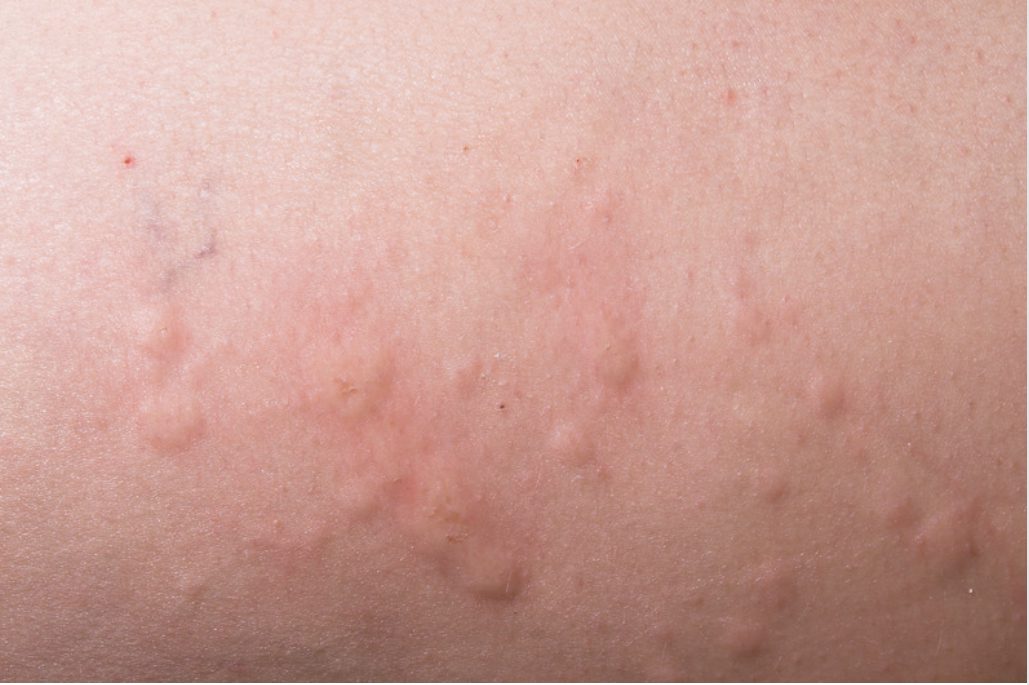
Hives can appear as round, red or pink welts and they may be either small or large. They can either show up alone or in a big group. Hives usually last just a few hours and itch. Unlike eczema, they’re short-lived and should go away within 24 hours. However, new hives can show up too, which might continue for weeks or longer. They also differ in that they can cause swelling of your lips or other areas on your body where they are found.
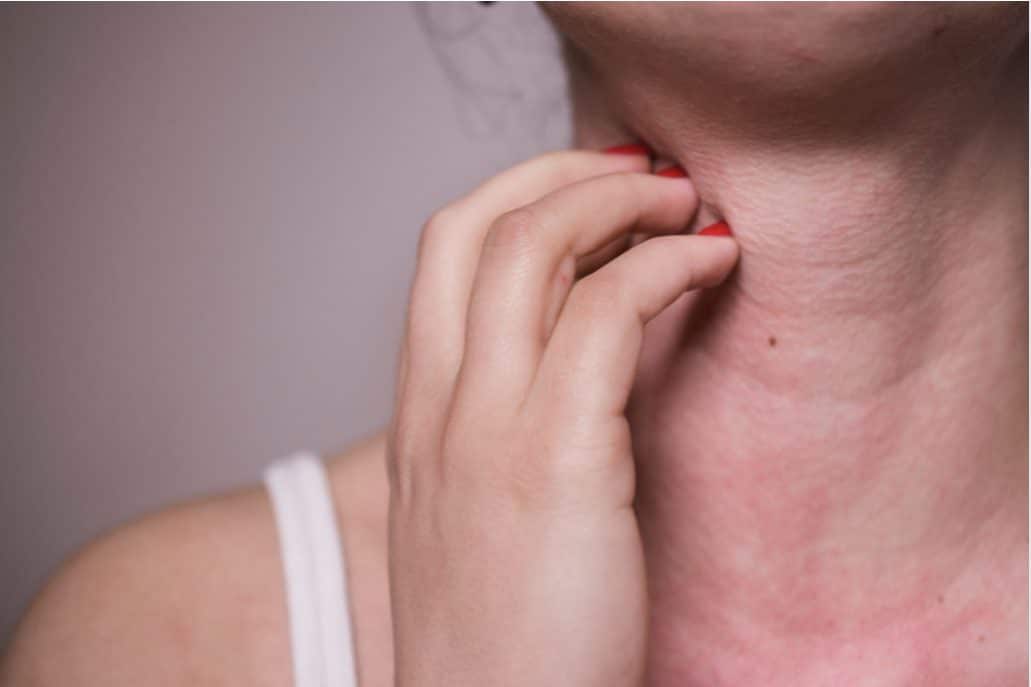
Allergies can cause some people’s eczema to flare up due to allergens like pet dander and dust mites. But lots of things can trigger eczema, including certain fabrics, soaps, and detergents. That means allergies may not be the reason your symptoms get worse.
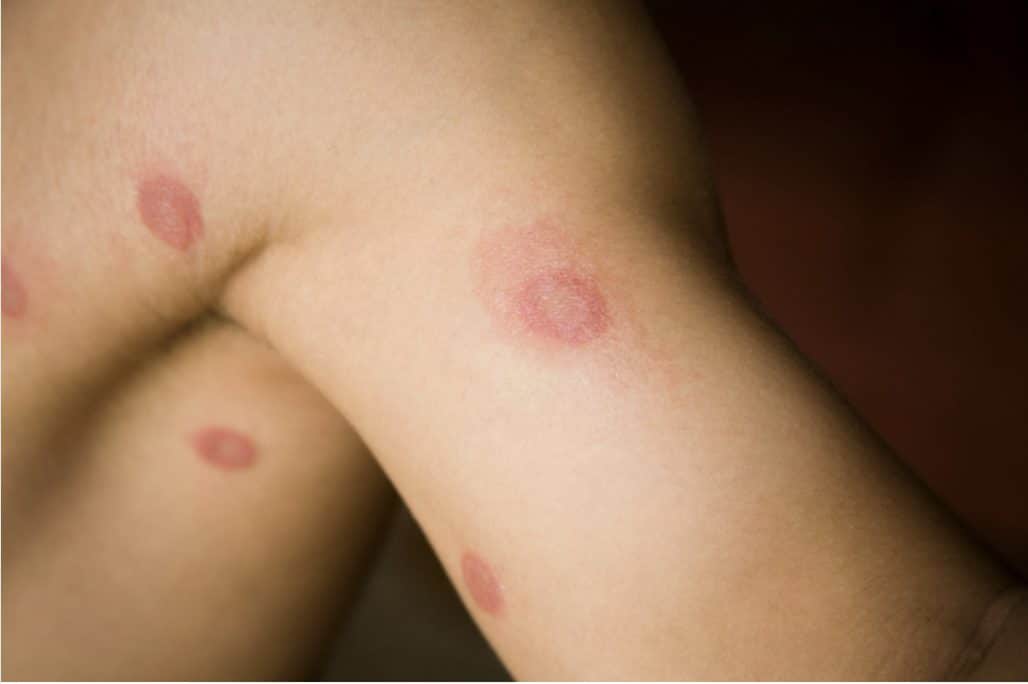
Ringworm, one of the most common types of fungal infections, can be passed to other people by direct contact with an infected person’s skin. This contagious infection is characterized by ring-shaped patches that will slowly enlarge on any part of your body. On lighter skin, these itchy patches might look pink or red. On darker skin, they might appear brown or gray. Ringworm patches usually have a wavy, raised border, but the center clears up first with treatment.
Acne is a skin condition that can take several forms, including Whiteheads, pimples, blackheads, nodules, or cysts. It is possible to have both eczema and acne at the same time, but usually not in the same area of the body. Eczema can be confused with acne, although the two are different.
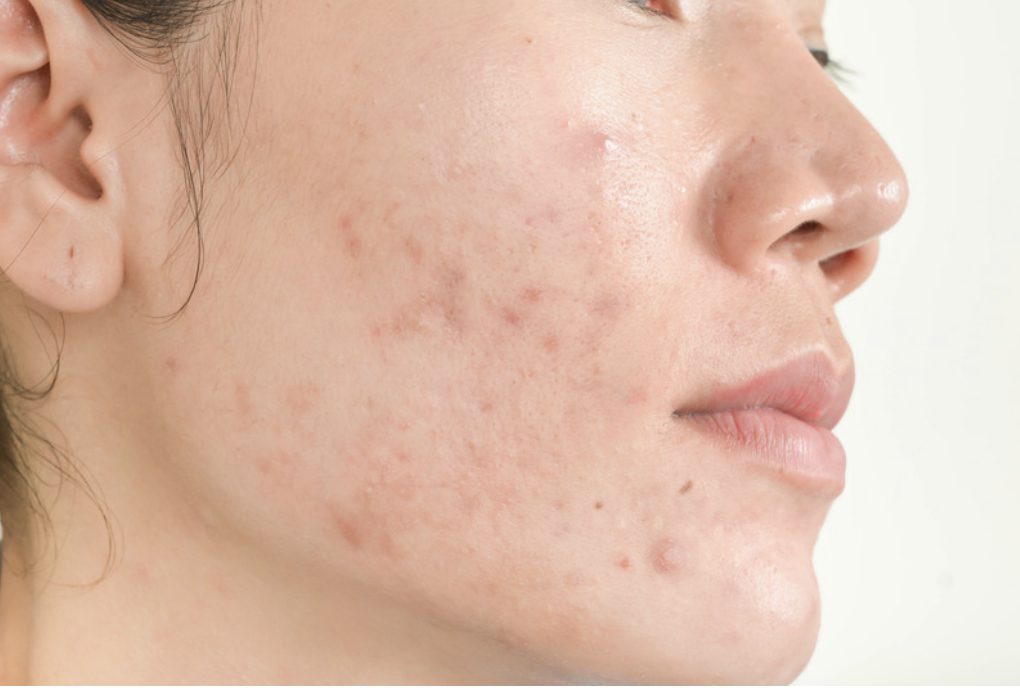
Cutaneous T-Cell Lymphoma is the most common form of this rare form of blood cancer. In its early stages, it can resemble eczema and may cause red, inflamed, itchy skin. If you have a rash that doesn’t seem to be getting better or that seems like it could be more serious than eczema, see a dermatologist just for peace of mind.
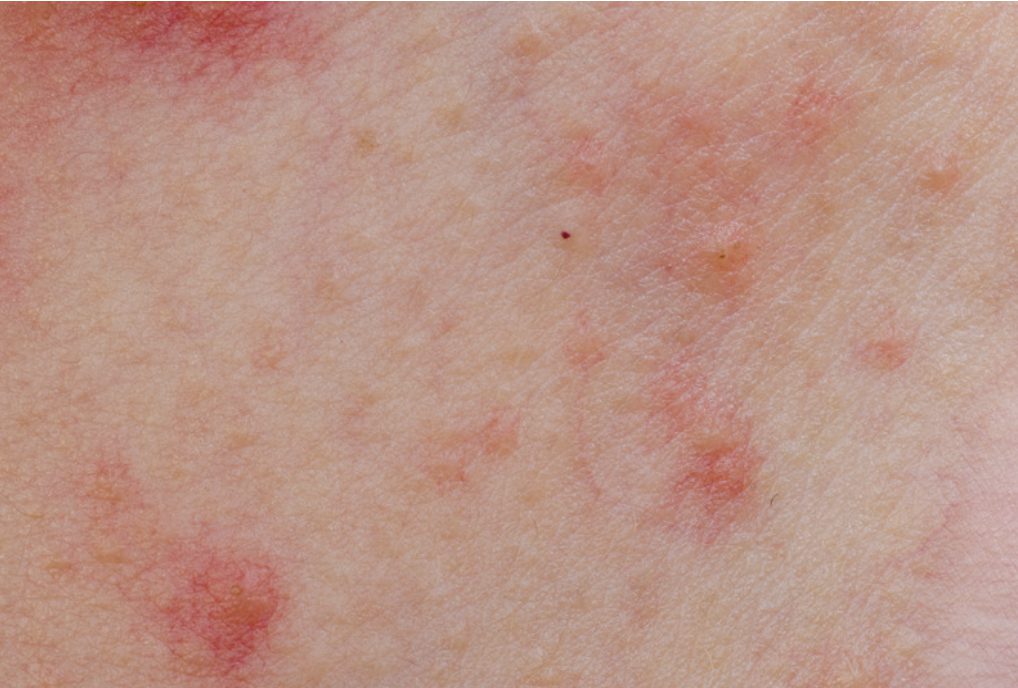
Netherton’s disease is a rare skin, hair, and immune system disorder. Symptoms that are first present at birth include red, scaly skin. Some of the other symptoms include outbreaks of red, circular scales, thin or fragile hair, and immune reactions such as hay fever, asthma, itchy skin, and eczema.
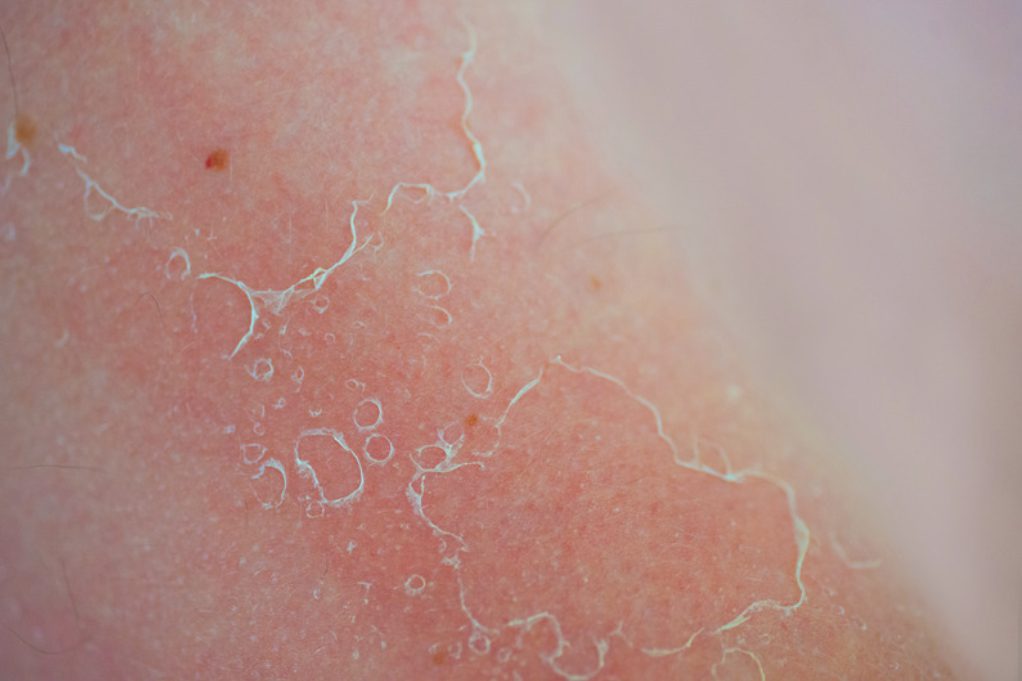
In conclusion, eczema and psoriasis are distinct skin conditions with different underlying causes, symptoms, and treatment approaches. Although both are chronic and can cause significant discomfort, a diagnosis is not the end of the world. With the right care plan, lifestyle adjustments, and consistent skincare, many people are able to successfully manage their symptoms and improve their quality of life.
Today, there are numerous treatment options available, along with a wealth of educational resources and supportive communities for those navigating chronic skin conditions. Understanding your skin’s needs is the first step toward long-term management and relief.
Your skin plays a vital role in protecting your body and maintaining overall health. Show it the care it deserves with a gentle, barrier-supporting routine — and choose products like Waxelene that nourish and protect without unnecessary irritants.





0 Comments